What is a CPTⓇ Code and How are They Used?
Current Procedural Terminology (CPT) codes are procedure codes that describe medical services provided by healthcare professionals. These codes are required for billing health insurance companies.
If billing on a CMS1500 form, the CPT code goes in box 24D. If you are providing a superbill to a patient, the CPT code should be included.

MNT Codes
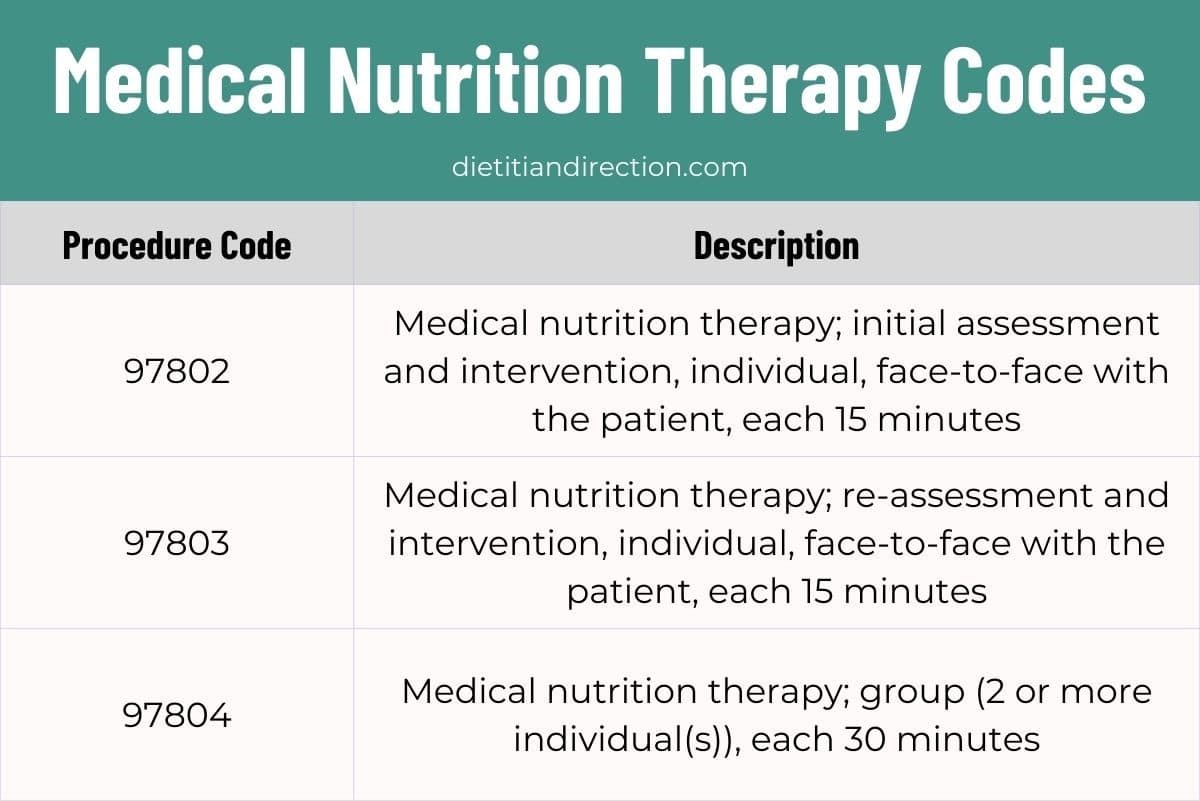
The Medical Nutrition Therapy, or MNT, codes are the go-to codes for registered dietitians when providing nutrition counseling. They include CPT codes 97802, 97803 and 97804.
CPT Code 97802
The description of CPT code 97802 is, “medical nutrition therapy; initial assessment and intervention, individual, face-to-face with the patient, each 15 minutes.” Let’s break this down one piece at a time.
Firstly, this code is used for Medical Nutrition Therapy (MNT). The Academy of Nutrition and Dietetics (AND) describes MNT as a specific nutrition service, used for the treatment of an illness, injury or condition, that involves an assessment, nutrition diagnosis, nutrition intervention and finally, nutrition monitoring and evaluation.
Therefore, MNT is not health coaching, providing general health information nonspecific to the patient, or reviewing food records. This is not to say these things cannot be part of an MNT appointment, but if these were the only things provided during a session, an MNT CPT code should not be used, as this is not MNT.
Secondly, this code is to be used for an individual. If MNT was provided in a group setting, CPT code 97804 should be used instead.
Thirdly, the appointment must be provided face-to-face with the patient. This does not necessarily mean the appointment has to be in-person, as this code can and should be used for telehealth, as well as in-person.
As far as we know, this is referring to the fact that the patient must be present during the appointment. If only the parent or caretaker is attending the appointment, not the actual patient, then this is not meeting the definition of the code. Per information from AND in the fall of 2023, the CPT Editorial Panel will discuss the definition of face-to-face at a future meeting, so more detailed information may come out in the future.
Finally, 97802 is a time based code and is billed for each 15-minute increment. So, if an initial appointment is 60 minutes long, it will be billed for 4 units. Rounding is allowed with this code and is done using the 8-minute rule.
Only time spent directly with the patient can be counted. Any time spent by the dietitian outside the appointment, including looking at medical records, documenting, researching or collaborating with other healthcare providers, cannot be counted.
CPT Code 97803
The description of CPT code 97803 is, “medical nutrition therapy; re-assessment and intervention, individual, face-to-face with the patient, each 15 minutes.” This code is to be used when follow up MNT appointments are performed.
Otherwise, this code is quite similar to 97802. This code generally pays out less than 97802.
CPT Code 97804
CPT Code 97804 is the third MNT code and is described as, “medical nutrition therapy; group (2 or more individual(s)), each 30 minutes.” This code is to be used when performing group MNT sessions.
This is a time based code, but note, it is based on 30 minute units rather than 15-minute units.
Frequently Asked Questions about MNT Codes
How Many Units Can Be Billed for CPT Codes 97802 and 97803?
Not all insurance companies or individual plans have the same limits on how many units can be billed for 97802 and 97803 during a single appointment.
For instance, many Aetna plans only cover 4 units per appointment, while other companies and plans may have a much higher limit. I, personally, have been paid for appointments that were 6 and even 7 units long.
Different dietitians will have different preferences on how long they like their appointments to be. Initial appointments are often scheduled for 60-90 minutes (4-6 units), while follow ups are often scheduled for 30-60 minutes (2-4 units). Again, this is just provider preference.
Can I Bill a Patient for 97802 More Than Once?
Part of the description of CPT code 97802 states that it is an initial assessment, so it is generally used once per patient. However, there are certain situations in which dietitians are wondering if they can use 97802 again. Using this code would be beneficial as it generally pays out more than 97803, but it should not be used unless appropriate.
Generally speaking, if a dietitian is meeting with a patient regularly or somewhat regularly, there should be no need to go back to using 97802. A change in insurance carrier or a change in fiscal year does not warrant using 97802.
Three Year Rule
Both the American Medical Association (AMA) and Centers for Medicare & Medicaid Services (CMS) state that for professional services, a “new patient” is someone that has not received services in the last 3 years. Based on this rule, if the patient has not been seen in three years or more, it would be appropriate to bill 97802.
Medicare Rules
Medicare states that 97802, “must only be used for the initial visit.” Code 97803 should be used otherwise, even when there’s a change in the patient’s medical condition that affects the nutritional status of the patient.
Medicare also notes that 97802 can only be used once a year, per patient. This is important to be aware of, especially if a patient saw another dietitian in the past. A claim could be denied if another dietitian already billed 97802 in the last year.
Professional Judgment
Per direct contact with AND in November 2023, they stated that not all payers may necessarily follow the 3 year rule and recommended contacting the payer directly. Frankly, insurance companies, with the exception of Medicare, most likely will not have specific rules regarding this issue. Ultimately, it is up to the provider to critically evaluate if the appointment should be considered an “initial assessment” or not.
The three year rule, in my opinion, is the best guidance we have for this situation. As with many things related to medical coding and billing, there is often no specific guidance in black and white.
Just like nutrition science, professionals may interpret billing and coding information differently. This is not legal advice and it is always best to err on the side of caution.
Other Codes Dietitians May Use
Dietitians may use other codes beyond the MNT codes, but it is advised to proceed with caution. Make sure you understand what the code means, how it can be billed and if it is part of your contract.
Some other procedure codes dietitians may potentially use are:
For more information about procedure codes and additional codes dietitians can use, see the post Dietitian CPT Codes – Nutritional Counseling & Beyond.
References:
CPT Overview and Code Approval
RDN’s Complete Guide to Credentialing and Billing: The Private Payer Market
